Infections and Fertility: The Silent Barrier to Parenthood
By Dr. G. A. Rama Raju, MBBS, DNB, PhD
Director, Krishna IVF Clinic, Visakhapatnam
Introduction
While hormonal and genetic factors are commonly recognized causes of infertility, infections represent a significant and frequently overlooked contributor.
A substantial proportion of global infertility cases are linked to infections, many of which are preventable with early identification. Timely testing and treatment can preserve fertility in many cases. Diseases such as sexually transmitted infections and maternal sepsis are key causes of female infertility and challenge women of reproductive age. However, effective medical care and increased awareness could prevent some infection-related infertility. Thus, proactive measures are critical.
Krishna IVF Clinic emphasises the following key message:
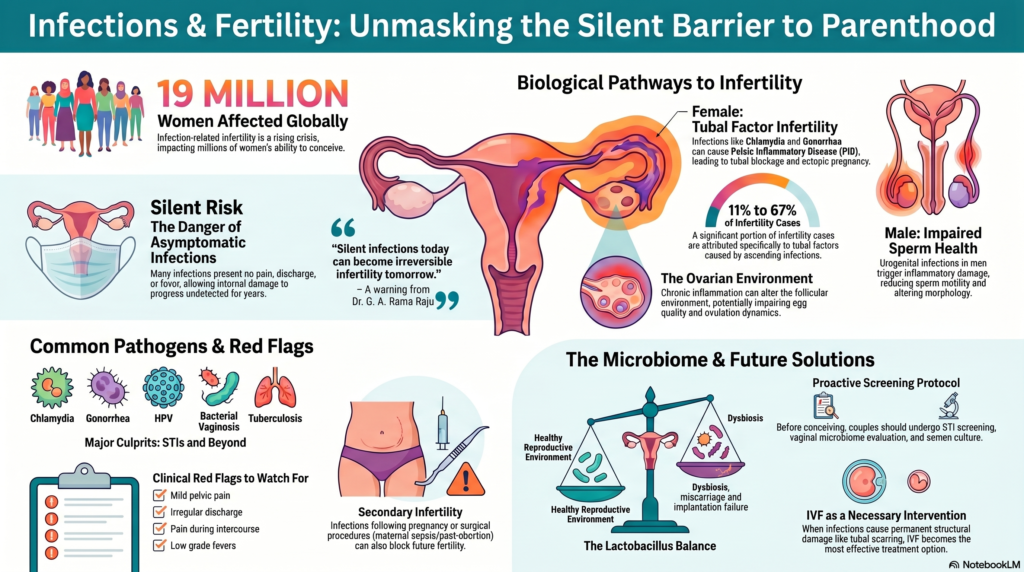
Understanding how infections impair fertility forms the basis for effective prevention and treatment. The following sections outline the specific biological pathways involved, thereby providing a framework for recognising where interventions can be targeted. Let us first examine how infections can affect different parts of the reproductive system:
Infections impact fertility through multiple biological pathways:1. Damage to Fallopian Tubes
• Sexually transmitted bacterial infections such as Chlamydia and Gonorrhea can move upward from the vagina or
cervix (the lower part of the uterus) into the uterus (womb).
• These infections can lead to Pelvic Inflammatory Disease (PID), a condition where infection causes inflammation of
the female reproductive organs.
• Lead to:
o Tubal blockage
o Scarring
o Ectopic pregnancy
Fallopian tube disorders account for approximately 11–67% of infertility cases.
2. Impact on Eggs and Ovarian Environment
• Chronic inflammation alters the microenvironment surrounding ovarian follicles.
• May impair:
o Oocyte quality
o Ovulation dynamics
• Emerging research suggests that imbalances in follicular microbiota may affect ovarian function. Patients may wish
to discuss microbiome testing with their healthcare provider, especially when considering fertility treatment. Early
identification and management of microbial imbalances could improve the ovarian environment and fertility outcomes.
3. Effects on Sperm Health
• Infections in the urinary and reproductive organs of men can:
o Reduce sperm motility
o Alter morphology
o Trigger inflammatory damage
Infectious agents (such as bacteria or viruses) in semen impair sperm’s swimming ability and shape. It’s also important to consider how infections can impact the uterus and implantation.
4. Endometrial and Implantation Failure
• Changes in the natural bacteria of the uterine lining affect:
o Implantation
o A disruption in the normal bacterial balance, especially the loss of Lactobacillus (a beneficial type of bacteria)
dominance, is linked with:
o Miscarriage
o Recurrent implantation failure
Common Infections Linked to Infertility
Sexually Transmitted Infections (STIs)• Chlamydia trachomatis
• Neisseria gonorrhoeae
• HPV, HSV
Many of these infections are asymptomatic, delaying diagnosis.
Genital Tract Infections
• Bacterial vaginosis
• Mycoplasma / Ureaplasma
• Tuberculosis (important in India)
According to a study published in 2015, Mycoplasma genitalium was identified in 16% of women with infertility in North India, while it was not found in women without infertility. Patients who have concerns about fertility may consider discussing the Mycoplasma test and monitoring with their healthcare provider. As research continues, evaluation may help address potential risks and offer reassurance.
Post-pregnancy or Surgical Infections
• Maternal sepsis can cause infertility after a previous pregnancy, leading to secondary infertility.
The Silent Nature of Infection
A significant challenge is that many infections remain undetected, complicating early intervention efforts.• No fever
Yet, internal damage continues.
As a result, infertility may only be recognised years after the initial infection.
This brings up an important question: Is infection-related damage to fertility always irreversible? To answer this, it is helpful to distinguish between early and late-stage consequences of infection.
Early Stage✔ Infection treated → fertility often preserved
Late Stage
Serious physical damage happens:
• Tubal scarring → often irreversible
• Severe damage to sperm may last a long time.
In such cases, in vitro fertilisation (IVF) is often considered an effective treatment. Alternative options, including corrective surgery, pharmacological therapy, or assisted insemination, depend on the extent and location of the damage and patient factors. A comprehensive evaluation with a healthcare provider determines the most suitable treatment.
Why Women Are More Vulnerable. Women are at increased risk for ascending infections within the reproductive tract and frequently present with asymptomatic infections.
Global data indicate a higher burden of infection-related infertility among women.Clinical Red Flags Patients Ignore
Patients often dismiss early warning signs:• Mild pelvic pain
• Irregular discharge
• Pain during intercourse
• Low-grade fever episodes
• Even a single untreated infection may have long-term adverse effects on fertility.
Modern Perspective: Microbiome & Fertility
Fertility is now understood to depend on more than just the presence or absence of infection. It also relies on maintaining a balanced reproductive microbiome (the helpful bacteria naturally living in the reproductive organs). A healthy reproductive tract is typically dominated by Lactobacillus species (beneficial bacteria).• An unhealthy reproductive microbiome is
characterised by the presence of harmful (pathogenic)
bacteria rather than helpful ones.
Even minor microbial imbalances can:
• Reduce IVF success
• Affect implantation
• Increase miscarriage risk
Given these considerations, patients should take proactive steps to help safeguard their fertility. Speak with a healthcare provider about screening for infections and assessing microbiome health early, even before trying to conceive, to reduce the risk of infertility related to infections.
Before Trying to Conceive• STI screening
• Vaginal microbiome evaluation
• Semen culture (if indicated)
During Infertility Workup
• Tubal patency testing
• Endometrial evaluation
• Testing for infections (including tuberculosis in India)
Krishna IVF Approach
Krishna IVF employs advanced infection testing methods and protocols, utilising highly sensitive assays such as PCR, capable of detecting low levels of infection that standard tests may overlook. These comprehensive tests screen for a broader spectrum of infections simultaneously, providing a more complete assessment of reproductive health. For patients, this approach supports faster, more accurate diagnosis, allowing for informed treatment decisions and the opportunity to optimise fertility preservation.• Fertility care that considers the microbiome
• Personalised treatment plans:
To maximise your chances of reproductive success, always consult with your healthcare provider about testing for and
treating possible underlying infections as part of any infertility evaluation or treatment plan. Actively addressing
infections is vital for preserving fertility.
