What is a Follicular Study?
A follicular study, also known as follicular monitoring, is essential for fertility assessment and treatment. It involves a series of ultrasound scans to track the development of ovarian follicles, which are tiny sacs in the ovaries where eggs mature. This study is crucial in understanding a woman's ovulation cycle. It is commonly used in both natural conception planning and assisted reproductive technologies like In Vitro Fertilization (IVF) or Intrauterine Insemination (IUI).
– Dr. G. A. Ramaraju DNB PhD, Consultant Krishna IVF Clinic

Why is a Follicular Study Important?
1. Ovulation Tracking: The primary purpose of a follicular study is to pinpoint the exact time of ovulation, which significantly increases the chances of conception, whether naturally or through assisted reproductive techniques.
2. Cycle Irregularities: It helps diagnose irregularities in the menstrual cycle and identify issues like the absence of ovulation (anovulation).
3. Medication Response: For those undergoing fertility treatments, a follicular study assesses how well the ovaries are responding to fertility medications.
4. Optimizing Fertility Treatments: It aids in determining the optimal time for procedures like egg retrieval in IVF or timing insemination in IUI.
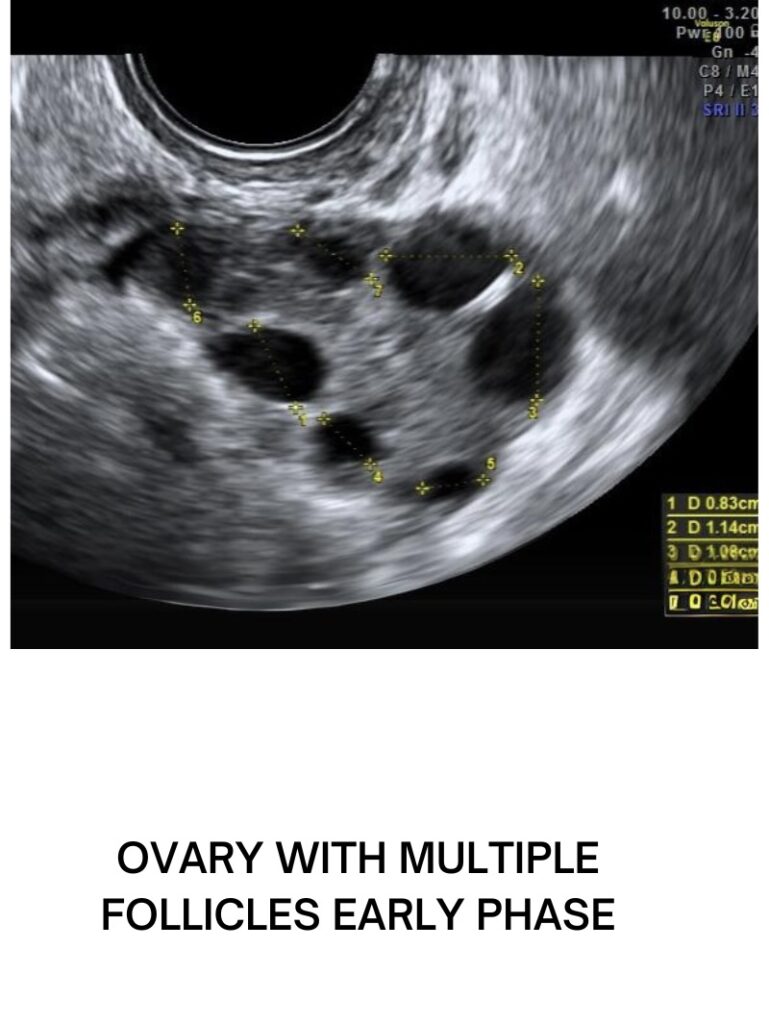
The Process of Follicular Study
A follicular study is performed through transvaginal ultrasonography, where an ultrasound probe is inserted into the vagina to get a clear view of the ovaries and uterus. Here’s what you can expect:
1. Baseline Scan: The process often starts with a baseline ultrasound scan, usually performed on the second or third day of the menstrual cycle. This scan provides information about the uterinelining and any cysts or follicles at the start of the cycle.
2. Monitoring Phase: Subsequent scans are performed every 1-3 days, depending on the individual’s cycle and the physician’s protocol. During each visit, the sonographer measures the developing follicles’ size and assesses the uterine lining’s thickness and pattern.
3. Identifying Ovulation: The goal is to track the growth of the dominant follicle(s). Typically, a follicle is considered mature and ready for ovulation when it reaches about 18-22 mm in diameter. The physician may also check for signs of impending ovulation, such as the LH surge (Luteinizing Hormone), if blood tests are being incorporated.
4. Post-Ovulation Scan: Sometimes, a scan is done after the expected date of ovulation to confirm that the follicle has ruptured, and ovulation has occurred.
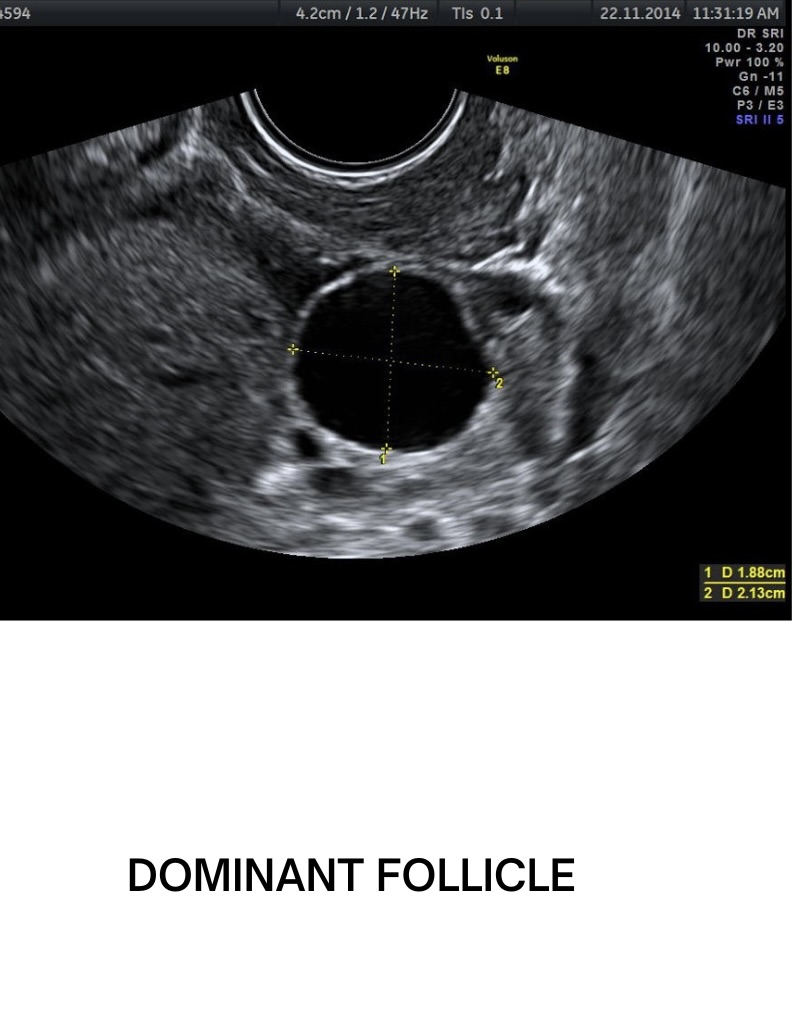

Understanding the Results:
The results of a follicular study can provide a wealth of information:
1. Follicle Size and Growth: Healthy follicle growth is about 1-2 mm daily, and tracking this growth helps predict ovulation.
2. Endometrial Thickness: The lining of the uterus should thicken in preparation for potential implantation. An endometrial thickness of around 8-10 mm is ideal during ovulation.
3. Ovulation Confirmation: On ultrasound, a collapsed follicle or free fluid in the pelvis can indicate that ovulation has occurred.

Factors Affecting the Follicular Study
Several factors can influence the outcomes of a follicular study:
1. Age: Ovarian reserve diminishes with age, affecting the number and quality of follicles.
2. Lifestyle: Stress, diet, and body weight can impact hormonal balance and ovulation.
3. Medical Conditions: Conditions like PCOS (Polycystic Ovary Syndrome) can result in multiple immature follicles and may require specialized monitoring.
What to Expect and How to Prepare
1. Frequency of Visits: Expect multiple visits to the clinic for scans. The exact number varies based on individual responses and treatment protocols.
2. Physical Discomfort: While generally not painful, some may find the transvaginal scans slightly uncomfortable.
3. Emotional Rollercoaster: The process can be emotionally taxing, given the anticipation and anxiety around the results. It’s essential to seek support and engage in stress-relief activities.
Conclusion:
A follicular study is a window into the intricate dance of hormones and events that lead to ovulation. It plays a pivotal role in fertility assessments and treatments, offering valuable insights into a woman’s reproductive health.
